Image credit: Pelvic Matters Zine team
Women’s health is underfunded and understudied. We explore how researchers across the Wellcome Sanger Institute are using advanced genomic tools to unpick the complexities of fundamental women’s health issues.
Despite women making up half of the population, scientific research significantly favours men’s health. In the UK, estimates indicate that only 2 per cent of medical research funding goes into studying pregnancy and reproductive issues, even though one in three women experience related issues.1
Female reproductive health covers a woman’s lifespan predominantly from puberty through to the menopause. During this time, many women experience painful conditions that impact their daily quality of life. Misdiagnosis, dismissal, mistreatment and stigma all compound these issues, significantly impacting women’s work, relationships, mental health and general wellbeing.
This blog examines how researchers at the Wellcome Sanger Institute are applying genomics to advance understanding of women’s health issues, including pregnancy complications and endometriosis.
Creating a spatial atlas of the cells in the reproductive system
New single-cell and spatial technologies are helping answer long-overlooked questions in women’s health. At the Institute, Group Leader Dr Roser Vento-Tormo’s team is searching for the causes of gynaecological and early pregnancy conditions. But to begin understanding how disease develops, they first needed to find out how the reproductive system is built and works in health. By tracking its cells across the lifespan and noting their characteristics – also known as atlasing – the team gained knowledge that now guides their disease research on larger cohorts.
The female reproductive tract develops through a very complex and coordinated process. It results in the formation of several organs – including the fallopian tubes, uterus, cervix and vagina – with distinct morphologies and functions. Dr Valentina Lorenzi, Staff Scientist in Roser’s group, used genomics to chart how the human reproductive tract forms before birth by creating a detailed map of its cells, including their location and communication throughout gestation. In a paper published last year, Valentina and colleagues used spatial transcriptomics and single-cell technologies to track how cells change over time and in different parts of the tissue.2 Capturing these rapid changes during development is essential, as many gynaecological conditions are believed to have their roots in these early developmental stages.
By studying the reproductive tract as a connected system rather than as individual organs across space and time, the team uncovered how different regions emerge from a shared starting point – called the Müllerian ducts. Their work showed that these regions are shaped by gradual changes in gene activity, rather than sharp boundaries. In particular, the researchers challenged previous assumptions about the HOX genes – which pattern the body during development – reshaping our understanding of how these genes direct the development of the human reproductive tract. They also revealed that supporting cells are key in guiding how tissues develop and signal to one another. Together, these insights offer a clearer picture of normal reproductive development and help lay the groundwork for understanding what may go wrong in gynaecological conditions such as endometriosis.

High-resolution image of the fallopian tube, uterus and ovary of a 21 post-conception week female sample. Image credit: Nature. 2025. DOI: 10.1038/s41586-025-09875-2
“The reproductive system is a particularly fascinating subject in developmental biology. Early in development, humans are sexually bipotent meaning the undifferentiated reproductive tissues have the capacity to develop into either male or female reproductive organs. Later, distinct reproductive structures develop through tightly regulated processes. This system undergoes rapid and dynamic changes over a short developmental window. The application of single-cell and spatial technologies has been critical for capturing these dynamics in high resolution. Together, these data have enabled the creation of a robust foundational reference map of reproductive organ development, which can be leveraged to gain deeper insights into the origins and mechanisms of reproductive disorders.”
Valentina Lorenzi,
Staff Scientist, Wellcome Sanger Institute
The team has now integrated developmental, paediatric and adult reproductive cell atlases to interpret large-scale genetic studies of female reproductive traits. Celeste Cohen, a PhD student working within the groups of Roser and Dr Carl Anderson, Head of the Human Genetics Programme and Senior Group Leader, is integrating genome-wide association study (GWAS) data with these cellular maps to better understand how genetic variation influences reproductive biology. By examining how different variants of the same gene are activated across cell types in the reproductive system – and at different stages of life – she can identify where these variants have the greatest impact, particularly those linked to key traits. This approach connects genetic variation to specific cell types, helping to pinpoint when and where important reproductive characteristics, as well as some gynaecological disorders, may arise.
“Reproductive systems are central to women’s health, given their fundamental role in hormonal regulation and their wide-reaching impact across the body. By mapping the development, regeneration and function of reproductive tissues using genomics, data-science and organoids, we are building a quantitative framework to understand how these systems work in health and disease. Looking ahead, the integration of large, deeply characterised cohorts, high throughput screenings and AI-driven analyses will allow us to dissect disease mechanisms at scale, bringing us closer to making female biology both predictable and clinically actionable.”
Roser Vento-Tormo,
Group Leader, Wellcome Sanger Institute
Understanding the immune system in pregnancy and associated complications
Pregnancy may be a natural part of life, but it profoundly challenges the body, placing exceptional physiological demands on the mother and triggering complex immune changes. The mother’s immune system faces a delicate task: accepting the genetically distinct foetus while still mounting enough defence to protect both herself and the developing baby from infection. When this balance is disrupted, it is believed to contribute to a range of pregnancy complications, including pre-eclampsia, preterm birth and gestational diabetes. Despite the clinical importance of these conditions, our understanding of how the maternal immune system adapts across pregnancy remains incomplete, in large part because the key tissues at the maternal-foetal interface are difficult or impossible to sample during ongoing pregnancy.
At the Institute, PhD student Sophie Hoffman in Group Leader Dr Emma Davenport’s group, is hoping to address this gap by using the maternal blood as a window into the immune dynamics throughout pregnancy, as the foetus grows and develops.

Sophie Hoffman, PhD student, working at her desk. Image credit: Haerin Jang.
The team has received blood samples from the Rosie Hospital in Cambridge, with well-defined timepoints across pregnancy, which will allow them to track immune pathways and cell type changes as pregnancy progresses. More specifically, they will be analysing gene expression data from the maternal blood to see what immune cells are present, and how and when they change in activity over time. They will also look for patterns that are different between people with and without complications, which in the future, could support early prediction of the outcome of people’s pregnancies.
They will also integrate genetic information with gene expression data to investigate the mechanisms underlying immune adaptation in pregnancy, using eQTL analyses. eQTLs – expression quantitative trait loci – are genetic variants that influence how strongly particular genes are switched on or off. By identifying eQTLs that operate during pregnancy, the team hopes to link inherited genetic variation to changes in immune gene activity in this biologically relevant context. Studying these effects directly in pregnant individuals will hopefully provide clearer insight into the pathways driving pregnancy complications, with long-term implications for improved prediction, prevention and treatment.
“Pregnancy places unique demands on the mother’s immune system, yet we still know surprisingly little about how the body adapts over the course of pregnancy. By tracking how the immune system progresses during pregnancy and linking this to genetic data, we hope to understand why some pregnancies stay healthy and others develop complications. This in turn will provide fundamental biological insights that could transform how pregnancy and associated complications are predicted, prevented and treated.”
Sophie Hoffman,
PhD Student, Wellcome Sanger Institute
Deciphering how ectopic pregnancy develops at the cellular level
Pregnancy begins with a dialogue between the cells of the mother and the embryo. In the first days, embryonic cells attach to maternal tissue and start changing it to support the formation of the placenta. This process normally takes place within the mother’s uterus, specifically in a specialised layer called the endometrium (the uterine lining). During this stage, cells of the embryo known as trophoblasts invade the endometrium, enabling the developing embryo to establish a connection with the mother and receive essential nutrients. In some cases, however, this complex process occurs outside the uterus – most commonly in the fallopian tubes – resulting in an ectopic pregnancy. In the UK, around one in every 90 pregnancies is ectopic.3 It is very hard to diagnose and can cause severe physical, mental and long-term reproductive issues. In advanced cases that cannot be treated medically, patients may need surgical removal of the affected fallopian tube, which can lead to rupture, heavy bleeding or even maternal death – and adds a significant psychological burden due to the loss of the pregnancy and a reduction in future fertility.
Researchers in Roser Vento-Tormo’s group are unpicking the dialogue between embryonic and maternal cells by studying the space where the mother’s and embryo’s cells interact inside the uterus in normal and ectopic pregnancies with single-cell and spatial resolution. Studying the tissue directly offers unique access to the process of trophoblast invasion, revealing a level of detail that has not previously been possible.
This project builds directly on the group’s previous work describing the cells present in the placenta during early pregnancy and how they talk to each other.4 Now they are generating a comparable cellular atlas of ectopic pregnancy in the fallopian tube. By comparing healthy versus ectopic sites where the embryo is found, they hope to identify the key events that make placenta formation healthy and the pregnancy successful in humans. Guided by what they find in the pregnancy tissue, the team will be collecting blood samples from larger numbers of people to try to identify signals which would allow for an early diagnosis of an ectopic pregnancy. They are receiving ectopic pregnancy tissue samples from the Rosie Hospital at Addenbrooke’s, plus eutopic pregnancy (pregnancy in the uterus) samples via the Human Developmental Biology Resource and the biobank from the Loke Centre for Trophoblast Research.
RELATED SANGER NEWS STORY
Human cell atlas study reveals how the maternal immune system is modified early in pregnancy
The first cellular map of healthy early pregnancy could help researchers understand miscarriages and preeclampsia by revealing how cells from the developing placenta interact with the mother's immune system.
One of the key angles of the project is to explore how the maternal immune system responds to the development of the placenta in the fallopian tube compared to the uterus. The uterus and the fallopian tubes contain different types of immune cells, and thus comparing pregnancies in these two tissues could tell us how immune cells in the uterus help healthy placenta formation. The team will be using their atlases of ectopic and healthy pregnancies to find out what is different and evaluate these differences in advanced in vitro models – mainly organoids, which are three-dimensional mini-tissues grown in the lab from patient cells that model different organs. For this, organoids modelling the placenta will be grown with immune cells that are normally found either inside the uterus or the fallopian tubes. They will be working with Cellular Services at the Institute, who will be generating placental organoids at scale, so that Roser’s team can change the conditions under which these cultures of organoids and immune cells are grown to try and model what they are seeing in ectopic pregnancy. All of these approaches will help build a clearer picture of what cells andsignalling mechanisms regulate the communication between the placenta and maternal immune system.
“This is an ambitious project, and we are already generating some really exciting data. Ectopic pregnancy is a condition where we understand very little about its pathology, yet it impacts nearly 2 per cent of all pregnancies worldwide and can result in significant maternal morbidity. Obtaining the appropriate samples is extremely difficult, so technologies such as single-cell and spatial transcriptomics help us maximise the amount of data from the limited tissue we have. Ultimately, the goal of this project is to build a comprehensive resource that uncovers key biological mechanisms underlying ectopic pregnancy pathology, which will lay the groundwork for follow - up studies that could lead to improved diagnosis or more targeted treatment in the future.”
Christina Kim,
MPhil Student, Wellcome Sanger Institute
Mapping the cells of the endometrium to better understand endometriosis
The endometrium is one of the most dynamic tissues in the human body, continuously rebuilding and sheddingduring a woman’s menstrual cycle. Despite this, the endometrium has not been studied in great detail during its normal cycling. At the Institute, Roser Vento-Tormo’s group has generated detailed single-cell profiles of the endometrium to map how different cell types change, and how the tissue repairs and rebuilds itself throughout the menstrual cycle.5,6 Building this atlas of the healthy endometrium has enabled the team to have a look at one of the most common gynaecological conditions – endometriosis.
Endometriosis is a condition that occurs when cells similar to the ones in the endometrium are found elsewhere in the body. This can cause inflammation, pain, scar tissue and infertility – and can be very debilitating. Around one in 10 women of reproductive age are affected by endometriosis, yet we do not understand what causes it and current treatments can come with major life-altering consequences.7
By comparing the endometrium in healthy versus diseased states, the team has been able to identify differences in how tissue and immune cells behave, which may help explain why the tissue does not function normally in people with endometriosis.
The team has set up a clinical network across Europe with clinics in Spain and Czechia to collect tissue samples from abnormal endometriosis growths outside the uterus, along with detailed information about the patients involved.
As part of this work, Postdoctoral Fellow, Dr Charlotte Cassie and her colleagues in Roser’s group are also developing in vitro organoid models that incorporate different cell types found in the endometrium to better mimic its biology. Using single-cell RNA sequencing and transcriptomic analyses, their work aims to improve the representativeness of these models in comparison with patient tissue data, creating scalable systems for studying disease progression and testing potential therapeutic interventions. Making these models more representative of real tissue could accelerate understanding of endometrial conditions, such as endometriosis, and help develop new ways of diagnosis and treatment, addressing a current significant problem in women’s health research.

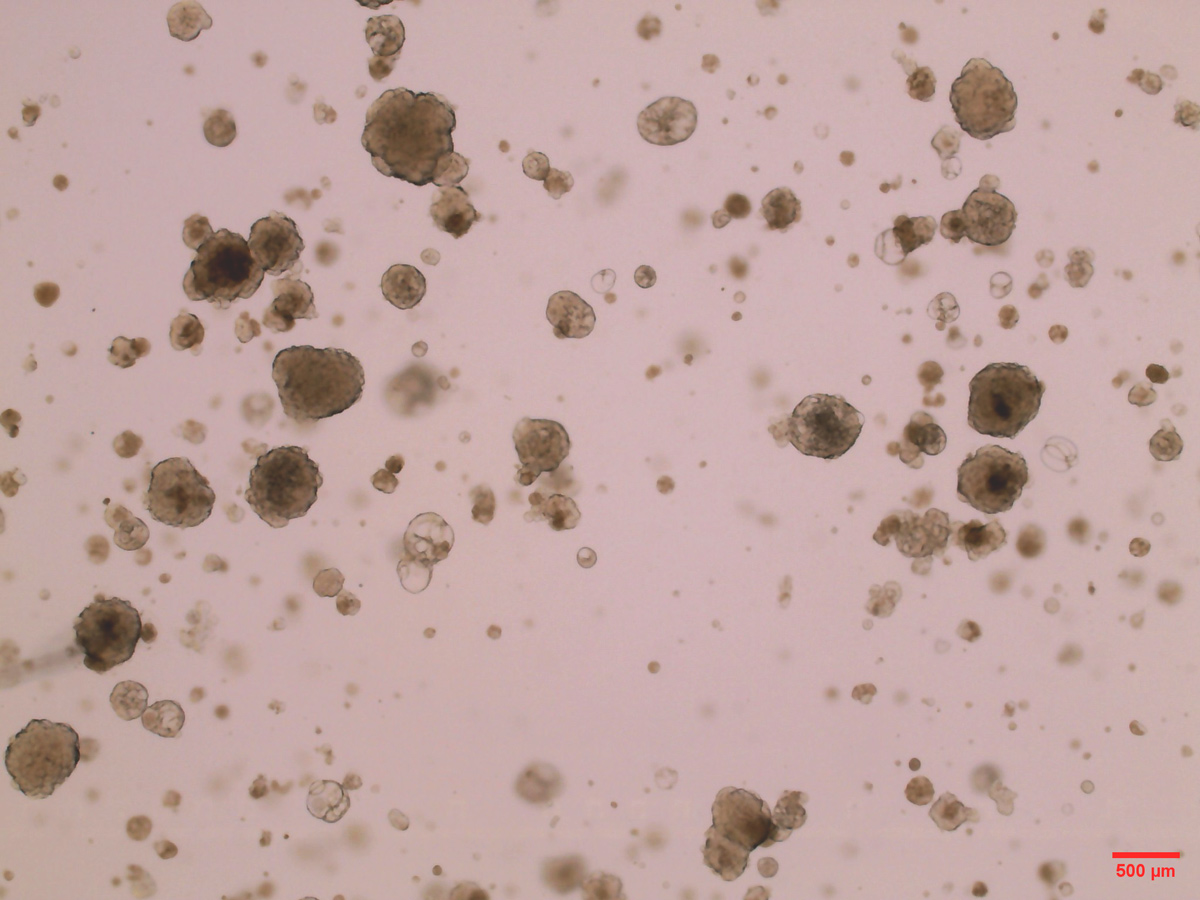
Endometrial co-cultures after hormonal stimulation. Image credit: Charlotte Cassie.
“The endometrium is constantly changing, yet for a long time we haven’t had the tools to really study it in detail. By generating representative in vitro models of the endometrium, we can look at how the different cell types of the endometrium interact. We can then apply this knowledge to start to understand what goes wrong in endometriosis as well as help establish non-invasive models, which could ultimately help patients get treatment quicker with more effective and beneficial outcomes.”
Charlotte Cassie,
Postdoctoral Fellow, Wellcome Sanger Institute
The team will use these advanced organoids to test potential cellular candidates that might be responsible for endometriosis, which they have previously identified in patient samples. They will then take a ‘lab-in-a-loop’ approach, where findings from patient tissues guide experiments in the lab, and the results are fed back to refine the next round of testing – accelerating the discovery of new therapies.
“Disease reshapes tissues and leaves clues behind, but these are often subtle and easy to miss within complex, heterogeneous samples. By first diving deep and mapping tissues in health and disease, we can define what is truly informative, and then build strategies to ensure those signals are measured when we scale up in large populations. The signal is there, the challenge is making sure that what is truly informative in the sample is actually being measured.”
Luz Garcia-Alonso,
Bioinformatics Lead, Wellcome Sanger Institute
Investigating menstrual fluid in large-scale populations
Approximately 1.8 billion people worldwide menstruate, yet menstrual fluid remains one of the most underused and poorly understood biological samples in medicine.8 Menstrual fluid is easy to collect and contains cells of the reproductive tract, such as the endometrium. This creates a rare opportunity for studying large numbers of these types of cells in a way that is easy for patients, especially in the context of some underexplored diseases.
To this end, Roser Vento-Tormo’s team is exploring the potential of menstrual fluid to study heavy menstrual bleeding, a condition affecting up to 37 per cent of those who menstruate.9 Despite its prevalence, our understanding of the underlying biology remains limited. Even the clinical definition of heavy menstrual bleeding is imprecise, relying on an arbitrary threshold of 80 ml of blood loss or more per cycle. The funding landscape for such research is a vicious cycle – we do not understand the basic biology, but many companies do not want to invest without knowledge of the basic biology. At Sanger, Roser’s group is part of a scientific programme funded by Wellcome Leap called the Missed Vital Sign. There are several known vital signs that can provide insight into our health, including blood pressure and core temperature. There are also suggestions that menstruation might be another vital sign that could indicate a lot about what is happening in women’s bodies.
As part of this programme, Dr Iva Kelava, Senior Staff Scientist in Roser’s group, is investigating heavy menstrual bleeding by analysing menstrual fluid in hundreds of participants recruited worldwide. More specifically, the team is profiling menstrual fluid using multiple approaches – including single-cell genomics, whole-genome sequencing and microbial profiling. This will create a complex dataset that captures genetic, cellular and environmental factors that contribute to the process of menstruation and might be involved in heavy menstrual bleeding. The team will integrate these different types of data using computational tools and, in collaboration with Group Leader Dr Mo Lotfollahi’s group, apply advanced artificial intelligence approaches to identify the different factors associated with heavy menstrual bleeding. Roser’s team will also grow menstrual-fluid-derived organoids that model key features of the endometrium – since that is the main tissue shed during menstruation – and use these to validate their findings and provide a platform for future therapeutic research. Overall, this work seeks to generate the first population-scale molecular reference of human menstrual fluid and use it as a tool for diagnosis, treatment design and ultimately, help break the cycle of silence and neglect surrounding menstrual health.
Raising awareness and recruiting for the BLEEDS study exploring heavy menstrual bleeding. Image credit: Iva Kelava.
Iva has been recruiting individuals at the Institute to non-invasively donate menstrual fluid samples using menstrual cups; these participants will serve as controls. The team is also collaborating with clinician Dr Miriam Baumgarten and research nurse Elena Otero Romero at Addenbrooke’s Hospital, who are helping to recruit individuals with diagnosed heavy menstrual bleeding. In addition, partnerships are being established with hospitals in Valencia, Chile and Singapore to collect samples from diverse populations, ensuring the study better reflects the full spectrum of human diversity.
“Menstrual fluid offers a unique, non-invasive window into the health of women, yet it has been largely ignored due to a lot of taboo and lack of investment. By studying it in detail using novel technologies such as genomics and organoids, we can begin to understand reproductive conditions such as heavy menstrual bleeding and bring long-overdue scientific attention to menstrual health.”
Iva Kelava,
Senior Staff Scientist, Wellcome Sanger Institute
Improving awareness of gynaecological health and conditions
In 2023, The Eve Appeal – the gynaecological cancer charity – estimated that only 7 per cent of people in the UK had good understanding of gynaecological symptoms before experiencing them.10 It was also found that just 5 per cent reported good knowledge of gynaecological cancers.10
To help address this knowledge gap, researchers in Roser Vento-Tormo’s group have developed Pelvic Matters. With illustrations from talented individuals across the Wellcome Genome Campus and beyond, the group has developed a collaborative zine on gynaecological health. The educational booklet covers topics such as female reproductive anatomy, the menstrual cycle, contraception, menopause and conditions like endometriosis, polyendocrine metabolic ovarian syndrome (previously known as polycystic ovary syndrome) and vulvodynia (vulval pain). By offering accessible, stigma-free content, Pelvic Matters encourages community members to better understand and advocate for the reproductive health of themselves or their loved ones.
The Pelvic Matters: A collaborative zine on gynaecological health. Credits: See final page of zine for artists, writers, reviewers and funders.
“It’s been a real privilege to be part of Pelvic Matters. Working on this has been both fulfilling and eye-opening, especially in showing just how many taboos still exist and how limited the general understanding of gynaecological health is. I hope this zine can be a starting point: helping raise awareness about this gap and encouraging people to engage more with their own gynaecological health, as well as that of those around them.”
Ana Paredes,
Postdoctoral Fellow, Wellcome Sanger Institute

Pelvic Matters team with their zine. Image credit: Valentina Lorenzi.
Find out more
- Vento-Tormo research group
- Anderson research group
- Sophie Hoffman's profile
- Davenport research group
- Alisha Dordi's profile
- Luz Garcia-Alonso's profile
- Lotfollahi research group
References
- Pure Unity Health. Addressing the Women’s Health Gap in the NHS. April 2025 [Last accessed: January 2026]
- Lorenzi V, Icoresi-Mazzeo C, Cassie C, et al. Spatiotemporal cellular map of the developing human reproductive tract. Nature. 2025. DOI: 10.1038/s41586-025-09875-2
- NHS. Ectopic pregnancy. August 2022 [Last accessed: February 2026]
- Vento-Tormo R, et al. Single-cell reconstruction of the early maternal–fetal interface in humans. Nature. 2018; 563: 347–353. DOI: 10.1038/s41586-018-0698-6
- Garcia-Alonso L, et al. Mapping the temporal and spatial dynamics of the human endometrium in vivo and in vitro. Nature genetics. 2021; 53: 1698–1711. DOI: 10.1038/s41588-021-00972-2
- Marečková M, et al. An integrated single-cell reference atlas of the human endometrium. Nature genetics. 2024; 56: 1925–1937. DOI: 10.1038/s41588-024-01873-w